Knee Osteoarthritis
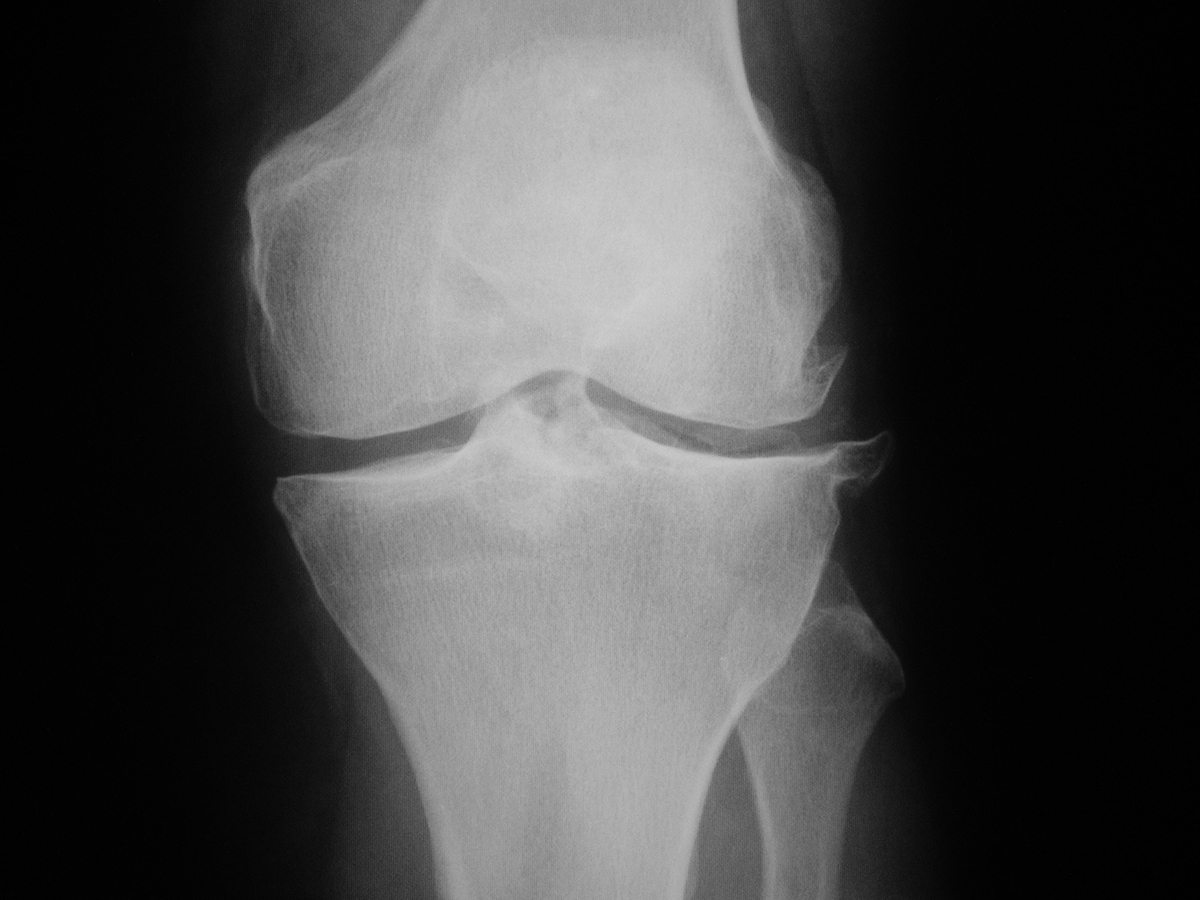
Cartilage is a pad that covers the joints facilitating friction and absorbing the impact that is generated. Osteoarthritis of the knee or gonarthrosis is a very prevalent pathology in trauma consultations and is caused by the wear and tear of the cartilage that covers the joint and that causes a malfunction of the same. This wear and tear can be generalized throughout the knee or located in a part of it, with the symptomatology being similar in both cases. This problem leads to a progressive loss of the quality of life of the person, who often has to modify their routines due to the limitations associated with this pathology.
The fundamental symptoms of this pathology are pain, joint stiffness, joint deformity and functional limitation:
- Pain is one of the first symptoms that manifest and is progressively established as the joint degenerates. The appearance is usually cyclical with pain-free periods and times with more pain or periods of crisis, which are associated with inflammatory processes of the joint. Initially it should be treated with analgesics, leaving the anti-inflammatories for episodes of acute crises. When oral treatments are not effective they can be treated with joint infiltrations (corticosteroids, hyaluronic acid, PRP…).
- Stiffness is another symptom associated with osteoarthritis of the knee. It is characterized by difficulty in the mobility of the knee after periods of inactivity, such as when getting up from a chair or in the morning when getting out of bed. These symptoms in premature phases disappear after a short period of activity, as if the joint required a warm-up prior to the activity, but can reappear if we perform long activities. In advanced stages the rigidity is felt constantly.
- In situations where the wear of the knee occurs asymmetrically, being the wear greater in one area of the knee than in another can give joint deformity. In these cases there is a deviation of the knee and an arching of the leg (genu varo) or an "X" arrangement of the legs (genu valgo).
- Functional limitation implies both a limitation of the range of motion of the knee, preventing activities such as squatting, and a progressive decrease in the perimeter of the gait. This can condition the decrease in daily activity and the abandonment of routines and other activities.
The establishment of these symptoms occurs progressively as the joint undergoes a greater degeneration of cartilage. The patient will notice greater rigidity, limited mobility, pain at a shorter distance from walking or of greater intensity that finally can no longer calm with usual analgesics.
Causes and how I can improve
There is a certain group of factors that favor the appearance of osteoarthritis in the knee:
- Excess weight
- History of knee injury whether traumatic, previous surgeries or knee cartilage diseases
- female
- Rheumatic diseases
- Elite sport or jobs with heavy load on the knees either by carrying weight or by working squatting.
The only variables that have been shown to be effective in slowing the progression of osteoarthritis are weight control and reduction and moderate physical activity. The cartilage receives all the loads of the body and if we decrease the body weight, that cartilage that is degenerated will have to support less loads, thus improving the symptomatology. It has been described that a 10% decrease in body weight can improve knee pain by about 50%. With regard to moderate physical activity, there is an improvement in muscle tone. This favors the stability of the joint and that the patella and the extensor apparatus of the knee work correctly. Activities that do not have excessive impact are recommended such as walking, trekking (according to level), pool exercises, bicycle or directed classes adapted to age and physical condition.
Treatment
Both oral and intraarticular treatments of collagen and / or hyaluronic acid should be oriented to the improvement of symptomatology, being effective especially in the initial stages of osteoarthritis. These treatments have no capacity for cartilage regeneration, as this is a tissue that has no regeneration capacity. They are considered supplements to treatment without clear evidence of their effectiveness, but that can sometimes help improve symptomatology.
When we cannot control the symptoms with standard analgesics and joint infiltrations and the patient's quality of life is impaired, it is time to consider surgical intervention. The intervention to be performed may vary depending on the cause and the age at which it occurs:
-
- Osteotomy: At younger ages with a leg deformity and monocompartmental osteoarthritis the indication may be an osteotomy, with the intention of aligning the limb and lengthening the life of the knee.
- Knee prosthesis. In case of an older age a knee prosthesis will be recommended, which depending on the type of osteoarthritis can be, unicompartmental if osteoarthritis affects only one area of the knee or total prosthesis if it affects 2 or 3 compartments of the knee. It is a surgery with good results in the short and long term. It requires a correct and intensive postoperative rehabilitation and realistic expectations of results that your specialist must explain before surgery.



